A Moment of Truth in the Pandemic
As the most ambitious pandemic-response initiative ever conceived, the COVID-19 Vaccine Global Access Facility is the best chance the world has to bring the pandemic to an end. But to succeed, COVAX requires broad international buy-in, based on the recognition that no one is safe until everyone is.

Vaccine Apartheid
Because a pandemic can be overcome only when it is overcome everywhere, embracing an every-country-for-itself approach would seem irrational. And yet, as the unseemly competition for vaccine doses indicates, that is exactly what many countries have done.
NEW DELHI – The American pharmaceutical company Pfizer and Germany’s BioNTech have announced that the COVID-19 vaccine they are jointly developing was more than 90% effective in early clinical trials. The news raised hopes around the world that life may soon return to pre-pandemic normal.
Those hopes may not last long. The announcement also sent governments scrambling to lay claim to vaccine doses, apparently realizing a bleak prediction: wealthy countries and individuals will monopolize early doses of any effective vaccine.
The COVID-19 Vaccine Global Access Facility (COVAX) – led by the World Health Organization, the Coalition for Epidemic Preparedness Innovations, and Gavi, the Vaccine Alliance – was established precisely to prevent this outcome. The COVAX Facility aims to accelerate COVID-19 vaccine development, secure doses for all countries, and distribute those doses fairly, beginning with the highest-risk groups. In other words, the facility was created partly to prevent hoarding by rich-country governments.
So far, more than 180 countries, representing nearly two-thirds of the world’s population, have joined. This includes 94 higher-income countries, all of which have made legally binding commitments. All will have access to the vaccines in the COVAX list, and pay for their doses individually. The 92 lower-income countries that are parties to the facility will receive their doses free of charge.
The COVAX plan would have the vaccine distributed in two phases. In the first phase, all participating countries would receive doses proportionate to their populations. It would begin with enough vaccines to immunize the 3% of their population at highest risk, especially frontline workers in health and social care. Additional doses would then be delivered, until immunization covers 20% of each country’s population – beginning with others most in danger from COVID-19, such as the elderly and those with co-morbidities.
In the second phase, vaccines would be delivered to specific countries based on how quickly the virus is spreading; whether other pathogens (like measles) are also spreading; and how vulnerable the country’s health infrastructure is to being overwhelmed. Given the constraints at work – the BioNTech-Pfizer vaccine, for example, must be administered in two doses three weeks apart, and only 1.35 billion doses, at most, will be produced by the end of next year – it is difficult to imagine a fairer system.
And yet there are major barriers to the system’s implementation. First and foremost, while China finally joined COVAX in early October, the United States has not.
Of course, given his “America First” approach, US President Donald Trump surprised no one by refusing to join. There is, however, reason to hope that President-elect Joe Biden will be more receptive. After all, Biden plans to re-join many international agreements from which Trump withdrew, and has already established a COVID-19 task force. Seth Berkley, the head of Gavi, the Vaccine Alliance, is set to hold talks with Biden’s team.
Meanwhile, China has been working aggressively and largely independently to develop and test its own vaccine. At least four candidates are currently undergoing Phase-3 trials. Though none are yet proven, Chinese officials have reportedly attempted to inoculate tens of thousands of people – possibly many more – outside the traditional testing process.
But there is another problem: COVAX participants are still competing to secure bilateral deals with pharmaceutical companies, as there is no rule against it. The United Kingdom, for example, has reserved 40 million doses of the BioNTech-Pfizer vaccine. Several other European governments have also placed orders, or are negotiating deals.
Moreover, the European Union has finalized a deal for up to 300 million doses. The US, with its population of 328 million, has ordered 100 million doses, with the rights to acquire 500 million more – a target so high that it smacks of an attempt to corner the market. Brazil – another COVAX participant – is also in talks with Pfizer, as are many others.
Within days of its announcement, Pfizer had sold more than 80% of the vaccine doses it will be able to produce by the end of next year to governments representing only 14% of the global population. In other words, if this is the first safe and effective vaccine to get to market, the vast majority of the world’s population will have almost no access to it.
Many other vaccine candidates – there are currently over 200, around 50 of which are in the clinical-trial phase – are also spoken for. Rich-country governments have already cut deals for privileged access to vaccines being developed by Moderna (which has also reported promising results from clinical trials), Johnson & Johnson, and AstraZeneca, among others, should these candidates make it through the approval process. Obviously, low-income countries do not have this option.
Because a pandemic can be overcome only when it is overcome everywhere, embracing an every-country-for-itself approach would seem irrational. And yet, as the unseemly competition for vaccine doses indicates, that is exactly what many countries have done. Unless we change course, global health apartheid will become increasingly entrenched and drive inequality to new heights. And the pandemic will still be with us. We will have merely added new problems to the one we didn’t solve.
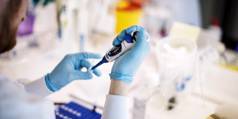
Could Vaccine Nationalism Prolong the Pandemic?
With multiple producers touting promising results in late-stage trials of COVID-19 vaccine candidates, the end of the pandemic finally seems to be in sight. But rather than work together to produce and distribute vaccine doses, some governments are taking an every-country-for-itself approach – raising serious risks not only for public health, but also for the economic recovery and geopolitical stability.
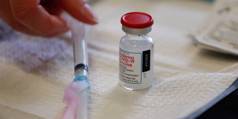
Can Poor Countries Avoid a Vaccine Bidding War?
For all of the good news about the arrival of safe and effective COVID-19 vaccines, the hard truth for the coming year is that global demand will outpace supply. Without a multilateral agreement to allocate doses globally, the road to recovery will be much longer than it otherwise could have been.
WASHINGTON, DC – The world has received the best possible gift for the coming year. The development of safe and effective COVID-19 vaccines in such a short time is something close to a medical miracle and portends an end to the crisis that dominated 2020.
But the pace at which we will end the pandemic depends on three factors. The first is the extent of continued compliance with recommended safety measures such as mask wearing, social distancing, crowd avoidance, and hand washing. The second factor is our ability to overcome the many logistical and distributional challenges of administering vaccines globally. And the third is access to vaccines for poorer countries. The pandemic will not be over until the coronavirus has been vanquished everywhere.
Some efforts are already underway to achieve this. For example, COVAX, a coalition of 172 countries (not including the United States), is seeking “to guarantee rapid, fair, and equitable access” to vaccines “for people in all countries.” Co-led by Gavi, the Coalition for Epidemic Preparedness Innovations, and the World Health Organization, it has already made arrangements with nine pharmaceutical developers to procure vaccines once they have been approved. So far, the European Union and individual EU member states have contributed the most to the effort – €850 million ($1 billion) to date – followed by the Bill & Melinda Gates Foundation and other major donors.
COVAX is seeking to raise $5 billion by the end of 2021 so that it can procure two billion doses. But even with a vaccine requiring only one dose (the current approved vaccines require two), two billion would not be enough to cover the developing world’s population. And while there is hope that producers in countries such as India can manufacture vaccines less expensively, the global supply will still fall far short of demand.
In addition to COVAX, there are also efforts to provide financing for poor countries directly. The World Bank, for example, has committed $160 billion to its client countries, and many other donors and philanthropic foundations have contributed in a similar fashion. Moreover, under the World Bank and the International Monetary Fund’s joint Debt Service Suspension Initiative (DSSI), 73 poor countries have been offered the opportunity to postpone debt-service payments until June 2021. As of early December, 45 countries had signed up for the program, with most of them freeing up funds equivalent to 0.1-2% of GDP.
While universal access to the vaccine is essential to overcome the pandemic, it is not clear that allocating more money to poor countries for vaccine purchases will actually enable them to obtain more doses, given the anticipated supply issues. Approved producers are already straining against capacity limits, and while there may be favorable surprises, increased demand (and thus the price at which the vaccine may be purchased) is unlikely to stimulate significantly higher production.
Moreover, many of the current contracts commit producers to sell at cost, with the quantities already specified. After those stocks are depleted, additional financing to countries pursuing unilateral purchases would likely result in a bidding war, thereby driving up the price and offsetting the gains to overall welfare.
To be sure, the companies that undertook the risk of pursuing a safe and effective vaccine deserve to be compensated for their efforts. As productive capacity increases, market forces should be allowed to provide incentives for innovation, development, and the creation of additional production facilities. But given the extent of demand for vaccines in 2021 is likely to exceed supply, further incentives for additional production cannot be expected to improve the supply-demand balance within the year.
And that is hardly the only concern. If some poor countries are sufficiently creditworthy, they may borrow more to finance vaccine purchases at the same time that the price for vaccines rises, leaving them with more debt but not a greater supply of vaccines than they otherwise might have procured.

Meanwhile, other poor countries that were already highly indebted are confronting debt-servicing difficulties that they would have faced even under normal economic circumstances. And some of those receiving DSSI support may simply use the freed-up funds to finance debt-servicing commitments rather than to purchase vaccines. To the extent that other creditors – such as private banks and major bilateral official lenders like China – get paid today, there will be fewer funds available later on for debt restructuring undertaken in conjunction with macroeconomic reforms.
These circumstances could result in there being fewer vaccines delivered to poor countries and greater rewards to creditors who received debt-service payments at the expense of those who offered DSSI forbearance. And in still other cases, the newly available funds might be directed toward other areas of government deficit spending instead of to vaccine purchases.
Given all of these complications, the best way to help poor countries obtain more doses is to reach an international agreement, presumably through COVAX and the WHO, to coordinate the allocation of available vaccines. The US is expected to rejoin the WHO after President-elect Joe Biden’s inauguration on January 20. Once that happens, a multilateral push to allocate vaccines efficiently to poor countries will have a high chance of success and should be pursued in earnest.
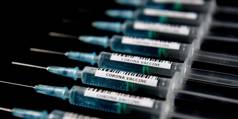
Designing Vaccines for People, Not Profits
For all the hope spurred by announcements of demonstrated efficacy in multiple COVID-19 vaccine candidates, there is still a long way to go to deliver on the promise of a universal, freely available "people's vaccine." As matters stand, national and private interests are trumping the principle of health justice.
LONDON – Recent announcements of demonstrated efficacy in COVID-19 vaccine trials have brought hope that a return to normality is in sight. The preliminary data for Pfizer/BioNTech and Moderna’s novel mRNA vaccines are highly encouraging, suggesting that their approval for emergency use is forthcoming. And more recent news of effectiveness (albeit at a slightly lower rate) in a vaccine from AstraZeneca and the University of Oxford has fueled optimism that even more breakthroughs are on their way.
In theory, the arrival of a safe and effective vaccine would represent the beginning of the end of the COVID-19 pandemic. In reality, we are not even at the end of the beginning of delivering what is needed: a “people’s vaccine” that is equitably distributed and made freely available to all who need it.
To be sure, the work to create vaccines in a matter of months deserves praise. Humanity has made a monumental technological leap forward. But the springboard was decades of massive public investment in research and development.
Most of the leading vaccine candidates prime the immune system’s defenses against the viral “spike protein,” an approach made possible through years of research at the US National Institutes of Health. More immediately, BioNTech has received $445 million from the German government, and Moderna has received $1 million from the Coalition for Epidemic Preparedness Innovations and more than $1 billion from the US Biomedical Advanced Research and Development Authority and the US Defense Advanced Research Projects Agency. The AstraZeneca-Oxford vaccine has received more than £1 billion ($1.3 billion) of public funding.
But for technological advances to translate into Health for All, innovations that are created collectively should be governed in the public interest, not for private profit. This is especially true when it comes to developing, manufacturing, and distributing a vaccine in the context of a pandemic.
No country acting alone can resolve this crisis. That is why we need vaccines that are universally and freely available. And yet, the current innovation system prioritizes the interests of high-income countries over those of everyone else, and profits over public health.
The first step toward a people’s vaccine is to ensure full transparency of the clinical-trial results, which would enable independent and timely assessments of safety and efficacy. The publication of scanty, preliminary data through corporate press releases is meant for financial markets, not the public-health community. This practice sets a bad precedent. While pharmaceutical share prices surge, health professionals and the public are left second-guessing the reported results. As more details about the flaws in clinical trial design and implementation for the AstraZeneca-Oxford vaccine emerge, so do the calls for open science and immediate sharing of protocols and results.
In addition, critical questions about the leading vaccine candidates remain unanswered. Responding to political and economic pressure in high-income countries, pharmaceutical companies are rushing their vaccine candidates across the finish line. Accordingly, they have designed their phase-three clinical trials to deliver the quickest possible positive read-out, rather than addressing more relevant questions such as whether the vaccine prevents infection or just protects against the disease. It also is unclear how long the protection will last; whether a given vaccine works equally well in young and old people, or in people with co-morbidities; and how the top candidates compare to one another (critical for designing effective vaccination strategies).
Moreover, national interests – especially those of developed countries – remain the dominant factor in vaccine rollout. While the international purchase and distribution platform COVAX represents a momentous step forward, its impact is being offset by massive bilateral advance-purchase agreements by rich countries that can afford to bet on multiple vaccines. For example, high-income countries have already bought close to 80% of the Pfizer/BioNTech and Moderna vaccine doses that will be available within the first year.
All told, rich countries have laid claim to 3.8 billion doses from different vaccine makers, compared to 3.2 billion (which includes around 700 million doses for COVAX) for the rest of the world combined. In other words, high-income countries have pre-ordered enough doses to cover their populations several times over, leaving the rest of the world with potentially too few to cover even their most at-risk communities.
At the same time, because the vaccine race is focused primarily on Western markets, some candidates are scarcely viable outside of a developed-country context. The Pfizer/BioNTech vaccine must be kept at -70ºC, which is colder than an Antarctic winter. Distributing this vaccine will create costly and complex logistical challenges, especially for low- and middle-income countries. Although other candidates – such as the AstraZeneca-Oxford vaccine – are stable at higher temperatures, it is notable that such glaring features of market discrimination are built into the first product to reach the approval stage.
Beyond national interest lurks the problem of even narrower private interests, which stem from an over-financialized biopharmaceutical innovation model. The business model for future vaccine development is already being sized up now that the pandemic has revealed the potential windfall for investors. But while they benefit from sky-rocketing stock prices, soaring capital gains, and dumping a company’s shares the same day it announces promising preliminary results in a clinical trial, delivering a people’s vaccine has become an afterthought.
The COVID-19 crisis is a perfect test of whether a more public-health-oriented approach to innovation and production will prevail in the years ahead. While Pfizer is sticking with the model of maximizing shareholder value, AstraZeneca has at least pledged not to profit from its vaccine “during the pandemic.” Yet, despite all the public investment that underwrote these innovations, the process will remain opaque, leaving one to wonder if AstraZeneca is actually ready to prioritize public health over profit and offer its vaccine at cost.
While the recent vaccine news has brought hope, it also has exposed the pharmaceutical industry’s broken business model, casting doubt on the prospects of delivering a people’s vaccine and achieving Health for All. Business as usual may allow us to scrape by in this crisis. But there is a better way to do things. Before the next pandemic arrives, we must recognize vaccines as global health commons, and start to reorient the innovation system toward symbiotic public-private partnerships governed in the public interest.
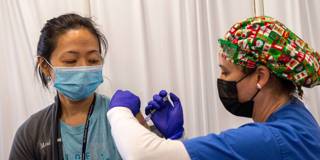
GENEVA – Now almost in its tenth month, the COVID-19 pandemic is still wreaking havoc on economies and lives around the world. But while the end of the crisis seems as far away as ever, the fact is that we are approaching a potential turning point. World leaders now have an opportunity to seal the deal on a global framework that puts international cooperation above vaccine nationalism in stopping the pandemic.
The moment of truth will be at midnight on September 18. That is the deadline for countries to join the COVID-19 Vaccine Global Access Facility (COVAX), an initiative launched by Gavi, the Vaccine Alliance, the World Health Organization, and the Coalition for Epidemic Preparedness Innovations. COVAX represents the best chance we have to provide people in all countries with rapid, fair, and equitable access to COVID-19 vaccines as soon as they become available. The initiative has already achieved an extraordinary scale, with more than 170 countries (representing 70% of the global population) already signaling their intent to join. At a time when most countries are undergoing unprecedented crises, governments are eager for solutions that will benefit everyone.
Nothing like COVAX has ever been attempted, and the short timeframe in which it has been assembled makes it all the more remarkable. If successful, this will be the first time that the international community has come together to ensure equitable and simultaneous access to new lifesaving pandemic interventions for rich and poor alike.
As we head into the fall, and COVID-19 continues to spread, the global death toll is approaching one million, with monthly economic losses estimated at $500 billion. Under these conditions, ensuring fair, universal access to vaccines is not only the right thing to do. It is also necessary if we are to bring the crisis to an end. Until everyone is protected, everyone will remain at risk of the disease, its adverse economic effects, or both.
As the only truly global approach available, COVAX’s importance cannot be overstated. Although there are more than 200 COVID-19 vaccines in development, and at least 35 clinical trials underway, the vast majority are likely to fail. Historically, candidate vaccines at the preclinical stage have less than a 10% chance of succeeding. And of those that do advance to the clinical trials stage, only around 20% will ultimately be approved. Given these odds, even wealthy governments that are currently negotiating bilateral deals with individual vaccine manufacturers cannot guarantee access to a vaccine on their own.
By contrast, COVAX is specifically designed to maximize the chances of success by investing in the development and manufacture of a large number of vaccine candidates at the same time. With the world’s largest and most diverse vaccine portfolio – which currently comprises nine candidates already in development and a further nine or more under evaluation – COVAX will act as a global insurance policy. Under this framework, member countries that have bilateral deals will still have vaccine access options in the event that those gambles fail, and the majority of countries that have no other options will be extended a critical lifeline.
COVAX’s initial aim is to have two billion vaccine doses available by the end of 2021, as that should be enough to protect high-risk/vulnerable populations and frontline health-care workers. But to hit that target, we first need the legally binding commitments of as many countries as possible.
After the sign-up deadline of September 18, the priority will be to complete the development and testing process to ensure that all forthcoming vaccines are both effective and safe. COVAX will need to put in place agreements with drug manufacturers, so that it can begin delivering vaccines at scale as soon as they are approved. And donor funds will be needed to subsidize the purchase of vaccines for low- and lower-middle-income countries.
But even with financial solutions in place, the process of distributing vaccines will pose significant challenges. The delivery of COVID-19 vaccines will be the single largest vaccine deployment the world has ever seen, and it will have to be executed at a time when misinformation (the “infodemic”) is threatening to undermine public confidence in vaccine safety.
Though the pandemic is far from over, we at least have a global solution in sight. COVAX represents the best hope that we have for bringing a prompt end to the crisis. When people look back and marvel at how quickly the scientific community and development practitioners responded to the COVID-19 threat, they will be able to point to the speed with which governments put aside national interests in the name of international cooperation and solidarity. Whatever specific moment future historians choose as the pandemic’s turning point, there will be little doubt that the creation and widespread adoption of the COVAX framework played an indispensable role in ending it.